Understanding the Glycemic Index

The Glycemic Index represents one of the most important concepts for anyone seeking to understand blood sugar management and make informed dietary choices. This numerical system ranks carbohydrates based on their immediate effect on blood glucose levels, providing valuable insight into how different foods affect the body after consumption. Foods with a high Glycemic Index cause rapid spikes in blood sugar, followed by equally rapid declines that can leave you feeling fatigued and hungry again soon after eating. In contrast, low Glycemic Index foods produce a slower, more gradual rise in blood glucose, providing sustained energy and better blood sugar control throughout the day.
Understanding the Glycemic Index empowers individuals to make smarter food choices that support stable blood sugar levels and overall metabolic health. While the Glycemic Index provides useful guidance, it should be considered alongside other factors such as portion size, food combinations, and individual responses. Combining high-GI foods with protein, healthy fats, or fiber can moderate their impact on blood sugar. Many whole foods, including most vegetables, legumes, and whole grains, fall into the low to moderate GI categories, while processed foods and refined carbohydrates typically rank highest. Incorporating more low-GI foods into your diet supports better energy levels, reduced cravings, and improved long-term metabolic health.
The Role of Dietary Fiber

Dietary fiber plays an extraordinary role in blood sugar management, offering benefits that extend far beyond simple digestion. Unlike other carbohydrates, fiber passes through the digestive system largely intact, providing bulk without contributing to blood glucose spikes. Soluble fiber, found in foods like oats, beans, fruits, and vegetables, forms a gel-like substance in the stomach that slows down the absorption of glucose into the bloodstream. This delayed absorption helps prevent the rapid blood sugar spikes that can lead to energy crashes and increased hunger. Insoluble fiber, present in whole grains, nuts, and vegetables, supports digestive health and helps maintain stable blood sugar levels through different mechanisms.
Research consistently demonstrates that high-fiber diets are associated with improved blood sugar control and reduced risk of developing type 2 diabetes. The recommended daily intake of fiber is approximately 25-35 grams for adults, yet most people consume far less than this amount. Gradually increasing fiber intake, while ensuring adequate hydration, can help the digestive system adjust and maximize the blood sugar benefits. Fiber-rich foods also tend to be more filling, which can support healthy weight management, another important factor in blood sugar regulation. Incorporating a variety of fiber sources throughout the day provides the greatest benefit and supports overall digestive health.
Regular Glucose Monitoring
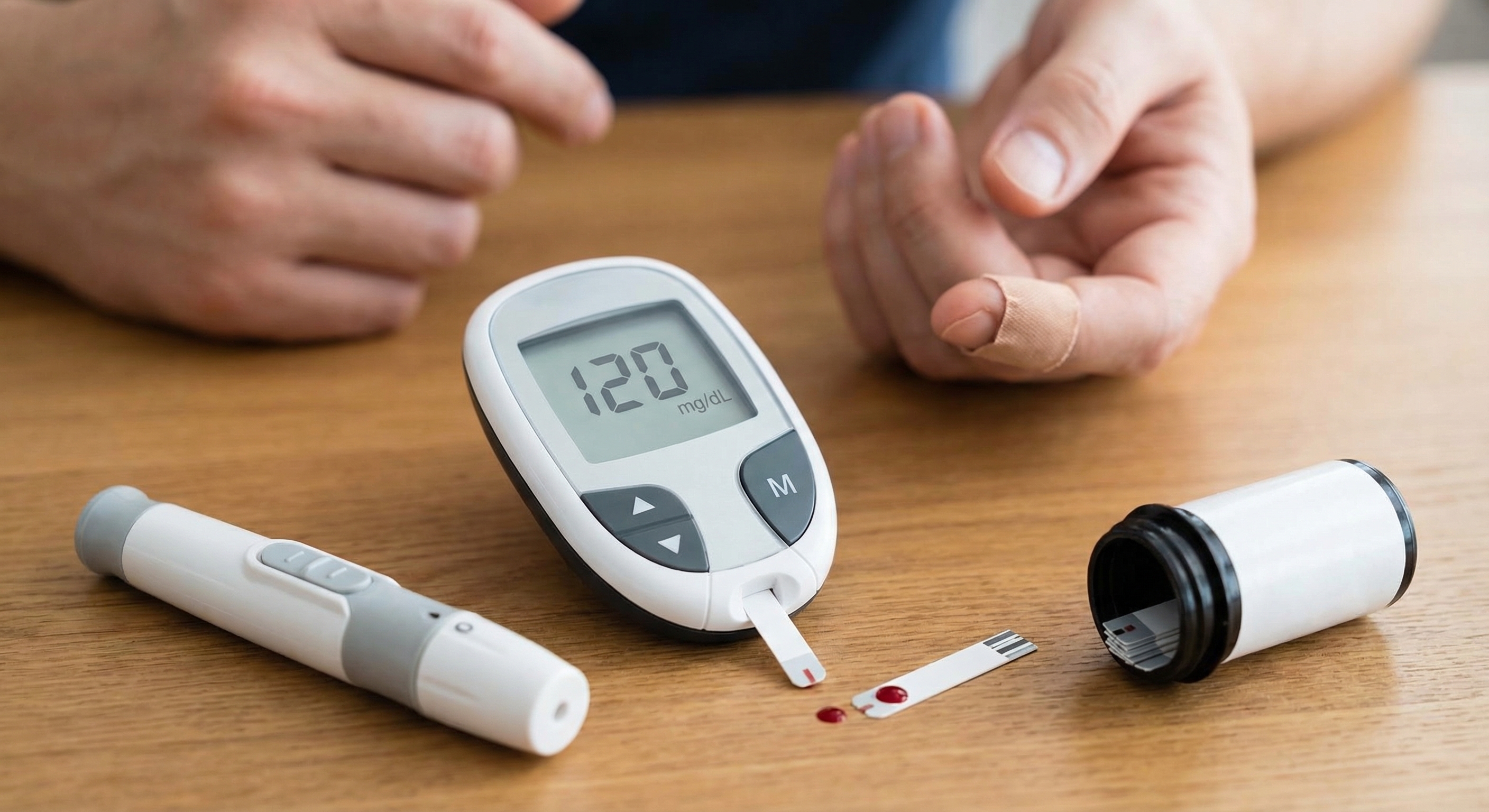
Regular glucose monitoring represents a cornerstone of effective blood sugar management, providing valuable information about how the body responds to food, exercise, and other factors. Understanding your blood sugar patterns allows you to make informed decisions about diet, physical activity, and other lifestyle factors that influence metabolic health. For individuals with diabetes, regular monitoring is essential for maintaining good glycemic control and preventing complications. Even for those without diabetes, awareness of blood sugar responses can provide insights into personal patterns and trigger points that affect energy levels and overall wellbeing.
Modern glucose monitoring technology has made it easier than ever to track blood sugar levels conveniently and accurately. Continuous glucose monitors provide real-time data and trend information, while traditional finger-stick meters remain a reliable option for many individuals. Understanding how to interpret glucose readings, including pre-meal and post-meal targets, enables more effective self-management. Working with healthcare providers to establish appropriate monitoring schedules and understand target ranges is essential for anyone managing blood sugar levels. Regular monitoring, combined with appropriate lifestyle modifications, supports better metabolic health outcomes.
Exercise and Insulin Sensitivity

Exercise stands as one of the most powerful tools for improving blood sugar control and overall metabolic health. Physical activity increases the body's sensitivity to insulin, meaning that cells become more effective at absorbing glucose from the bloodstream. This improved insulin sensitivity persists for hours or even days after exercise, contributing to better blood sugar control throughout the day. Both aerobic exercise and resistance training offer significant benefits, with each type providing unique advantages for metabolic health. Regular physical activity also supports weight management, reduces cardiovascular risk factors, and improves overall fitness.
The American Diabetes Association and other health organizations recommend at least 150 minutes of moderate-intensity aerobic activity per week, combined with two or more days of resistance training. Even shorter bouts of activity, such as walking after meals, can help moderate blood sugar spikes. For individuals taking blood sugar-lowering medications, exercise timing may need to be coordinated with medication schedules to prevent hypoglycemia. Starting with modest exercise goals and gradually increasing intensity and duration helps ensure sustainability. Finding activities that you enjoy increases the likelihood of maintaining regular exercise habits over the long term.
Hydration and Blood Sugar

Proper hydration plays a surprisingly important role in blood sugar regulation, yet it is often overlooked in discussions about metabolic health. When the body is dehydrated, the concentration of glucose in the bloodstream increases because there is less available water to dilute it. Additionally, dehydration triggers the release of stress hormones that can further elevate blood sugar levels. Staying adequately hydrated supports kidney function, which helps the body eliminate excess glucose through urine. Research has shown that increased water intake is associated with better blood sugar control and reduced risk of developing hyperglycemia.
The ideal amount of water intake varies based on individual factors including body size, activity level, and climate, but general recommendations suggest approximately eight glasses per day as a starting point. Water is the best choice for hydration, while sugary drinks and excessive caffeine can actually worsen blood sugar control. For individuals with diabetes, paying attention to hydration is particularly important, as high blood glucose levels can lead to increased urination and further dehydration. Making conscious efforts to maintain good hydration habits supports overall metabolic function and contributes to better blood sugar management.